Sub-Saharan Africa carries 24% of the global disease burden, but has access to only 3% of the world’s health workers. There is roughly one doctor for every 5,000 people across the region. The WHO recommends one per 1,000. That gap is not a statistic you can solve by training more doctors. Closing it through conventional means would require decades of medical school expansion, infrastructure investment, and health workforce development, which most African health systems simply don’t have the resources to accelerate. What is happening instead, right now, in Lagos, Nairobi, and Johannesburg, is something different. Artificial intelligence is being deployed not as a future promise but as a live, production-grade tool that extends the reach of overstretched clinicians, catches diseases earlier, reaches patients in places where no specialist will ever work in person, and does so on the devices already in people’s pockets.
This article is for you; whether you’re an investor tracking where Africa’s most consequential technology is being built, a health professional curious about the tools reshaping clinical workflows, an entrepreneur evaluating a gap in the market, or simply someone who wants to understand why the healthtech story coming out of Nigeria, Kenya, and South Africa is one of the most important technology narratives of this decade. These three markets were chosen deliberately. Together, they represent the continent’s three largest healthtech ecosystems in terms of funding, startup density, patient reach, and regulatory maturity. The companies profiled here are not theoretical. They are deployed, they have patients, and several of them are already reaching populations at a scale that would have been inconceivable a decade ago.
Why AI Is Transforming Healthcare in Africa: The Context You Need
Before you look at individual companies, you need to understand the structural conditions that make African healthcare AI both urgent and genuinely distinctive from anything being built in the US or Europe. The numbers are stark. Africa bears 24% of the global disease burden but has just 3% of the world’s healthcare workforce, a ratio that has not meaningfully improved in the past decade.
In Nigeria, the doctor-to-patient ratio sits at approximately 1:2,500. While in rural Kenya, it reaches as low as 1:16,000 in some counties.
Families across the continent pay 25–40% of their income out of pocket for healthcare, pushing millions into poverty annually. Only 15% of rural clinics use electronic health records (cities reach 45%), meaning most patient data doesn’t exist in any form that technology can act on.
What makes AI specifically powerful in this context, not just digitisation generally, is its ability to extend the reach of a single clinician to thousands of patients simultaneously without that clinician being physically present. Diagnostic AI can identify tuberculosis in a chest X-ray, detect birth asphyxia from a newborn’s cry, or flag cardiovascular risk from a mobile-captured vital sign, all in facilities where the nearest specialist may be hundreds of kilometres away.
The investment signal confirms what the technology is demonstrating clinically. African healthtech raised $224 million in equity funding in 2025, a 232% year-on-year increase, crossing $200 million for the first time since the 2021-2022 boom.
The regulatory environment is evolving alongside the investment. Nigeria’s NAFDAC is developing specific AI-guidance for medical devices. Kenya’s Digital Health Act of 2023 created the first formal legal framework for digital health on the continent. South Africa’s SAHPRA is building evaluation pathways for AI-based medical devices.
🇳🇬 Nigeria: AI Healthtech in Africa’s Most Populous Market
Nigeria has 220 million people, a severe doctor shortage, and one of Africa’s most active startup ecosystems. It is also where some of the continent’s most creative healthcare AI is being built, driven by founders who have lived the healthcare access problem personally and are building solutions that reflect that lived understanding.
Helium Health
Helium Health is the most comprehensive health infrastructure platform operating in Africa. Its core product is an AI-powered hospital management system and electronic health record (EHR) platform designed specifically for the operational realities of African hospitals: intermittent connectivity, variable staff technical literacy, and the need to integrate billing, clinical records, pharmacy, and lab management into a single workflow.
The platform serves over 500 health facilities across Nigeria and West Africa, processing millions of patient records and clinical transactions. Furthermore, Helium Health integrates AI for patient flow optimisation, insurance claims processing, and clinical decision support, meaning clinicians at a Helium-connected facility have access to data-driven insights that were previously available only at well-resourced private institutions.
The company’s Series B funding positions it as the dominant player in the hospital digitisation space in West Africa. Its acquisition of Kangpe (one of Nigeria’s early telemedicine platforms) shows that Helium is building toward a full-stack health ecosystem rather than remaining a point solution for hospital administration.
Honest Limitation: Helium Health’s model is enterprise-focused; it serves hospitals and clinics that have reached a minimum threshold of operational complexity. Community health centres, rural primary care facilities, and the most underserved clinics in Nigeria’s 36 states remain largely outside its current reach.
Ubenwa
Ubenwa is arguably the most globally recognised Nigerian AI health tool, and the one that most powerfully illustrates what constraint-first AI design looks like. The platform diagnoses birth asphyxia, a leading cause of newborn death and disability worldwide, responsible for approximately 900,000 deaths annually, by analysing a newborn’s cry through a standard smartphone microphone.
No specialist equipment. No radiologist. And, no neonatologist. Just a phone and an AI model trained on cry acoustic patterns.
Co-founder Charles Onu developed the concept from the premise that a newborn’s cry is a vital sign that deserves systematic clinical analysis. The Gates Foundation has backed the platform, and it has been deployed in clinical settings across Nigeria and other African markets. Consequently, Ubenwa addresses the specific problem of birth asphyxia detection in exactly the zero-specialist, zero-infrastructure environments where the disease burden is highest.
Honest Limitation: Audio quality from very basic phones can affect diagnostic accuracy. Environments with significant ambient noise create additional challenges that the team is actively addressing through model iteration.
Plato Health
This is one of Nigeria’s most-watched emerging AI health companies, having raised $1.4 million in pre-seed funding in early 2025, backed by Google for Startups and angel investors from Tesla. Plato Health’s AI-driven platform enables users to monitor and manage chronic conditions such as diabetes and hypertension from home using smart medical devices, addressing a massive, largely unmanaged chronic disease burden in Nigeria’s urban population.
Nigeria has one of the highest rates of undiagnosed hypertension in the world, with millions of people living with elevated blood pressure that they’ve never had measured. Moreover, Plato Health’s home monitoring model removes the clinic visit as a prerequisite for chronic disease management, a genuinely significant design choice in a country where specialist appointments can mean a half-day commute.
Honest Limitation: The availability and affordability of smart medical devices remain barriers for Nigeria’s lower-income populations. The platform currently skews toward urban, smartphone-equipped users, not yet the hardest-to-reach populations.
Remedial Health
Remedial Health tackles a problem that is less visible than diagnostic AI but arguably as consequential: access to medicine. It is a B2B pharmaceutical supply chain platform that uses data intelligence and demand forecasting to improve drug availability across Nigeria’s fragmented pharmacy network.
The platform raised a $12 million in Series A funding and has demonstrated that predicting medicine stock-outs and optimising procurement reduces the all-too-common scenario of patients being told their prescribed medication is unavailable. Field Intelligence, a related supply chain play, supported over 3,200 community pharmacies across Kenya and Nigeria by June 2024, improving health outcomes for more than 1.5 million patients. Remedial Health applies a similar logic: fix the supply chain, and you improve health outcomes at scale without a single clinical interaction.
Honest Limitation: The patient-facing impact of a supply chain platform is indirect and harder to measure than diagnostic or telemedicine tools; important, but less visible to impact investors who want clear clinical outcome metrics.
MDaaS Global
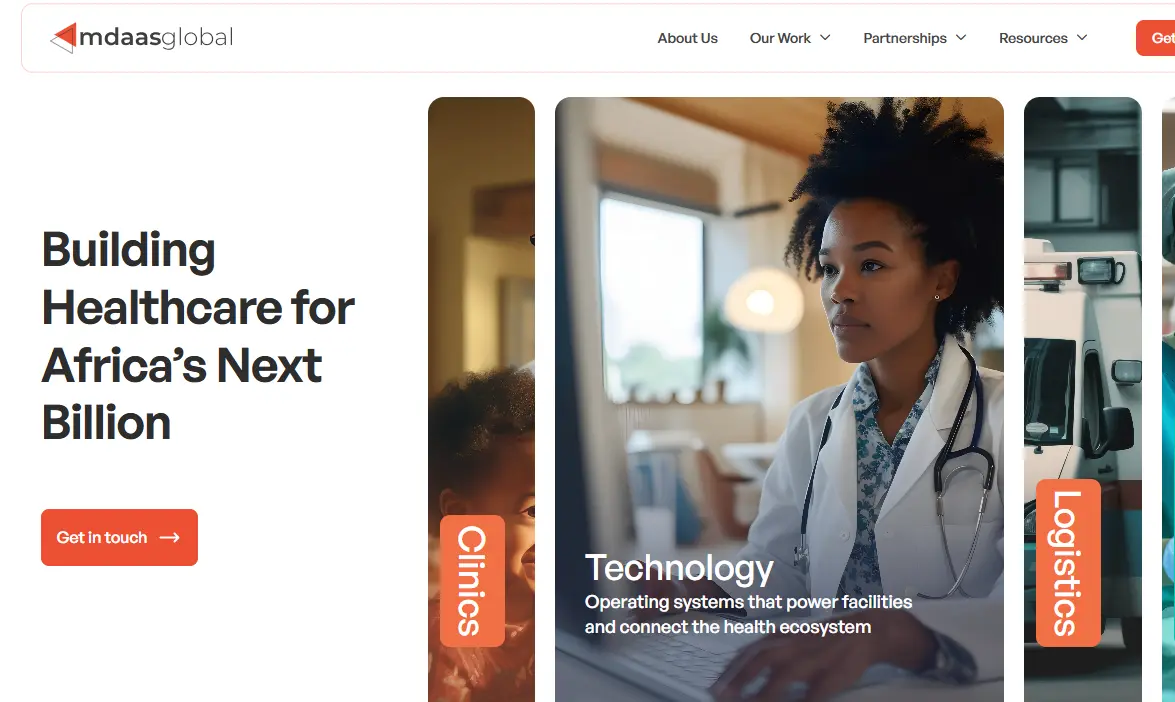
MDaaS Global takes a different approach from purely software-based plays. It builds affordable diagnostic centres in underserved Nigerian communities (Tier 2 and Tier 3 cities that private hospital chains don’t serve), combining physical diagnostic equipment with AI-assisted diagnostic tools, staff training, and operational technology.
Its Series A-funded model has demonstrated that high-quality diagnostics can be delivered profitably in markets previously considered too small or too poor to sustain a diagnostic centre. Furthermore, MDaaS has partnered with government health programs to integrate its centres into public health infrastructure; the kind of government alignment that unlocks patient volume at a scale private-only models rarely achieve.
Honest Limitation: The physical infrastructure model limits the speed of expansion relative to pure software plays. Building and equipping a diagnostic centre takes time, capital, and local operational management that a software update doesn’t.
Nigeria Ecosystem Snapshot
Nigeria’s AI healthtech ecosystem is maturing through a combination of deep local startup talent, growing government digitisation ambitions (particularly through the National Health Insurance Authority), and the sheer scale of the addressable market. The 2025 funding decline in Nigeria’s equity markets reflects normalisation after a 2021 peak, not ecosystem collapse. For AI healthtech specifically, the opportunity is expanding as NAFDAC develops its AI medical device guidelines and as hospital digitisation accelerates.
🇰🇪 Kenya: AI Healthtech in Africa’s Innovation Laboratory
Kenya punches above its population weight in African tech. With a mobile-first population, M-Pesa’s deeply embedded payment infrastructure, a government that has been more digitally progressive than most African peers, and an established startup culture that produces globally competitive products, Kenya has become the continent’s most important testing ground for AI health tools.
Nairobi alone attracted $536 million across 10 deals in 2025, accounting for 54.2% of all startup funding on the continent. Kenya’s healthtech sector is gaining traction specifically, and the regulatory environment is among Africa’s most innovation-friendly.
Ilara Health
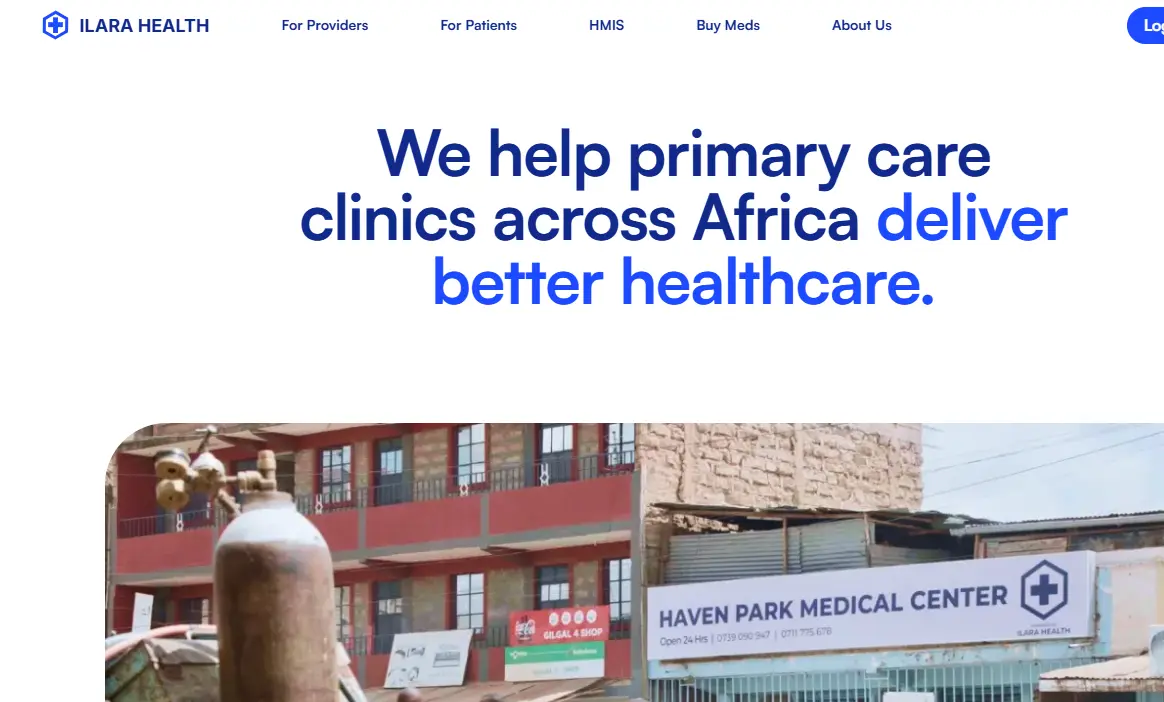
Ilara Health is one of the most important infrastructure plays in East African healthcare. Founded in 2019, it brings affordable AI-powered diagnostic devices and software to informal clinics and community health workers across Kenya, the facilities that serve the majority of Kenyans but have historically had access to almost no diagnostic technology. Its model is distinctive: rather than selling equipment outright, Ilara provides devices through a financing arrangement that community clinics can afford, combined with a software layer that integrates AI diagnostic capability and health information management.
Ilara Health uses AI to detect respiratory illnesses from the sound of a cough, one of several AI diagnostic applications integrated into its platform. It serves over 3,000 clinics across Kenya, meaning that a clinic in a rural county that previously had to refer every patient requiring diagnostics can now offer on-site AI-assisted diagnostics. Additionally, Brookings has specifically cited Ilara Health as an example of how African-built AI health infrastructure can extend clinical capability in genuinely resource-constrained settings.
Honest Limitation: The hardware distribution model creates unit economics challenges at scale. Financing arrangements for clinics with irregular cash flows require careful portfolio management and patient capital from investors.
Jacaranda Health
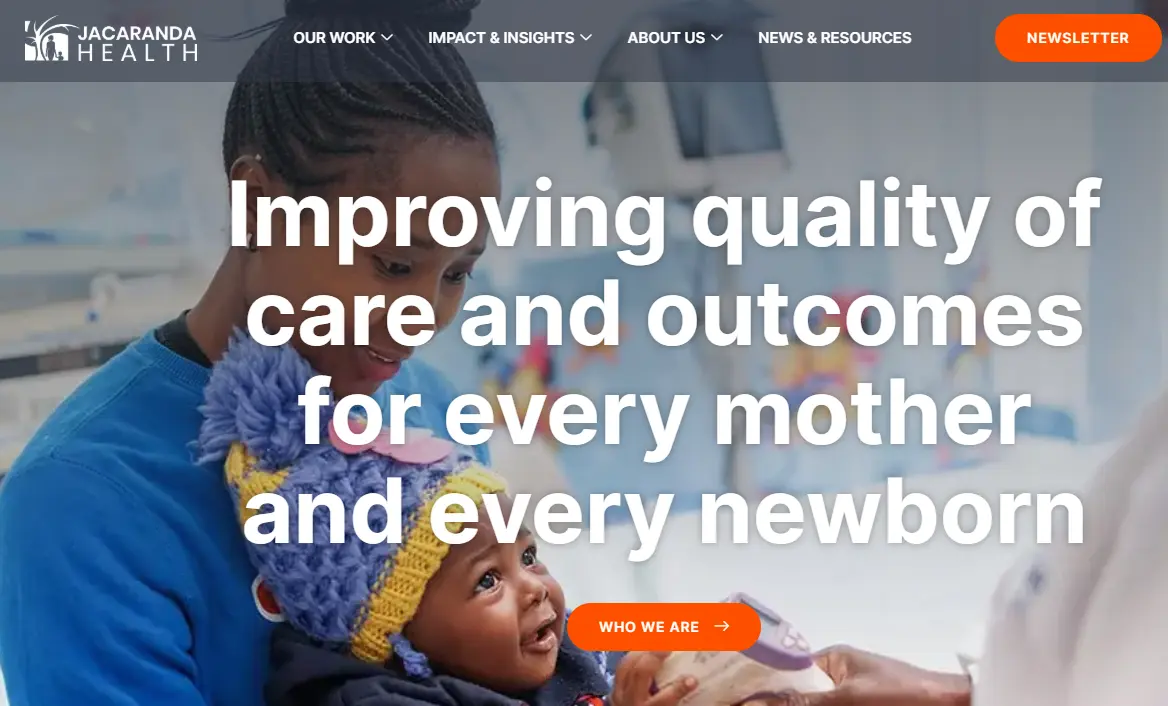
Jacaranda Health’s PROMPTS system is one of the most evidence-backed maternal health AI interventions on the continent. The platform sends personalised, AI-generated SMS health guidance to expectant and new mothers; advice calibrated to their specific gestational stage, health history, and risk profile. It works on basic phones with no data connection required, meaning it reaches exactly the population it’s designed for: women in rural Kenya for whom a smartphone app is neither accessible nor affordable.
The outcome data is compelling. Jacaranda Health and Google are collaborating on an initiative involving new handheld ultrasound devices and leveraging AI, a 2024 partnership that signals the platform is deepening its clinical capability beyond SMS-based guidance toward actual diagnostic hardware. The PROMPTS system has reached over 500,000 mothers across Kenya and operates in partnership with government health programs; the public sector alignment that gives it legitimate reach at a national scale.
Honest Limitation: SMS-based delivery, while accessible, limits the interactivity of the guidance compared to app-based alternatives. As smartphone penetration among Kenyan women increases, the platform will need to evolve its delivery model accordingly.
Zuri Health
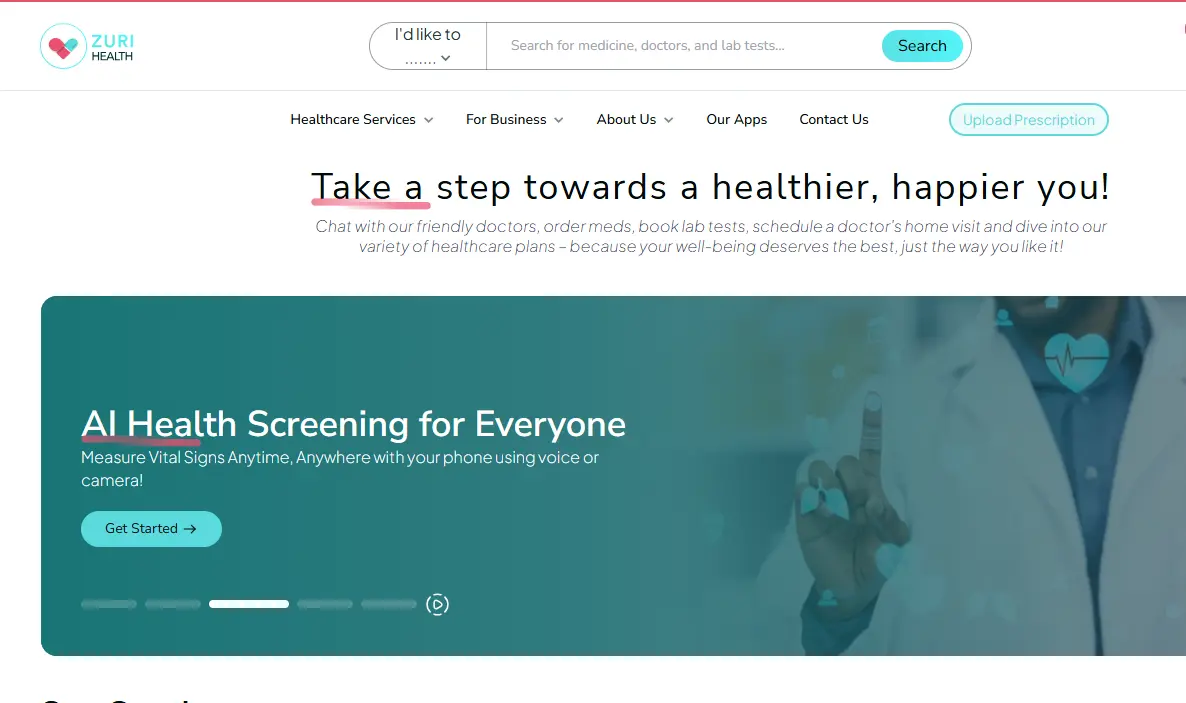
Zuri Health is East Africa’s most comprehensive AI-powered telemedicine platform, covering Kenya, Uganda, and Tanzania. Its distinctive technical feature is a video-based AI solution that uses photoplethysmography signals to analyse facial video and screen and monitor cardiovascular health metrics, including blood pressure, cholesterol indicators, and HbA1c. Zuri Health utilises a video-based AI solution to screen and monitor biometric parameters and cardiovascular health metrics, including blood pressure, total cholesterol, and HbA1c, a genuinely innovative application of computer vision to cardiovascular screening that doesn’t require any hardware beyond a smartphone camera.
Zuri provides on-demand doctor consultations alongside this AI triage capability, creating a full-stack telemedicine experience that begins with AI-assisted screening and escalates to human clinical review where needed. Consequently, patients who previously couldn’t access any medical consultation can now receive an AI-screened cardiovascular assessment and a doctor’s opinion in the same session.
Honest Limitation: The platform’s user base skews urban. Rural connectivity limitations continue to limit access for populations with the fewest alternative care options.
Flare (Emergency Response)

Flare addresses one of Kenya’s most acute and least-discussed health crises: emergency medical response. Nairobi has a documented emergency response gap, an uncoordinated network of private ambulances, public services with limited capacity, and hospitals with no real-time visibility into which emergency resources are available. Flare’s AI platform aggregates this fragmented emergency resource landscape, connecting patients to the nearest available ambulance, hospital, and emergency responder in real time.
The platform has processed thousands of emergency dispatches and partners with private hospitals and insurers who need reliable emergency routing for their members. Furthermore, Flare creates a data layer on top of Kenya’s emergency response system that didn’t previously exist, enabling analysis of response times, geographic gaps, and resource allocation that can inform policy decisions.
Honest Limitation: Flare is currently focused on Nairobi. Extending the model to peri-urban and rural Kenya requires a different density of emergency resource partners than currently exists outside the capital.
Kenya Ecosystem Snapshot

Kenya’s AI healthtech story is shaped by three forces working together: M-Pesa’s payment infrastructure (which enables health payments in ways impossible elsewhere), the Digital Health Act (which created the first clear regulatory framework for AI health tools), and a startup culture that produces globally competitive technical talent. The Smart Africa Alliance, comprising over 40 African countries, has developed frameworks for cross-border interoperability in digital health, and Kenya is among the most active participants in shaping that agenda.
🇿🇦 South Africa: AI Healthtech in Africa’s Most Developed Market
South Africa has the most developed healthcare infrastructure on the continent, and the most complex structural challenge. A two-tier system separates the 16% of the population covered by private medical aid (which funds world-class private hospitals) from the 84% who depend on a chronically underfunded public health system.
AI is attacking this problem from both ends simultaneously, improving efficiency in the private sector and extending reach in the public sector. South Africa reclaimed leadership in both equity funding ($643M, +41% YoY) and equity deal count (85 rounds, +27% YoY) in 2025, confirming that investor confidence in South African technology has meaningfully recovered.
Envisionit Deep AI
Envisionit Deep AI is South Africa’s most significant domestic AI diagnostic company and one of Africa’s 20 most promising startups to watch, according to African Business magazine. It provides AI-powered medical imaging analysis, specifically designed for the South African public health system’s radiology backlog.
South African public hospitals have a severe shortage of radiologists, meaning X-rays and scans routinely wait days or weeks for interpretation. Envisionit Deep AI’s platform delivers preliminary AI reads that prioritise urgent cases, enabling radiologists to work significantly more efficiently. Envisionit Deep AI is redefining healthcare access by turning diagnostics into predictable, high-quality systems, elevating healthtech from a niche service to a foundational layer of public health infrastructure.
Honest Limitation: The platform requires existing radiology hardware to function. In facilities without imaging equipment, which describes most rural public clinics, the AI has nothing to analyse.
Vula Mobile
Vula Mobile addresses one of South Africa’s most persistent structural healthcare problems: the specialist referral bottleneck. Rural and peri-urban healthcare workers regularly encounter patients who need specialist opinions that are hours away by road and months away by appointment. Vula Mobile provides a secure smartphone platform where healthcare workers submit structured patient information, images, and clinical notes to remote specialists across 14 clinical specialities, and receive expert guidance typically within hours.
The platform has over 5,000 registered healthcare workers across South Africa and has been used by doctors, nurses, and community health workers for cases ranging from ophthalmology to orthopaedics. Furthermore, Vula has won multiple global health innovation awards and has been cited by the WHO as a model for technology-enabled specialist access in resource-constrained settings. The AI layer assists in triage, helping route cases to the right speciality and flagging cases requiring urgent specialist attention before they reach the queue.
Honest Limitation: The platform depends on specialist availability and willingness to engage via the app. At scale, specialist response capacity becomes the binding constraint rather than the technology itself.
Zoie Health
Zoie Health is a women’s health platform founded by individuals with deep clinical knowledge combined with market understanding, a combination that the best current generation of African health founders increasingly bring to their work. It provides AI-assisted primary care, mental health support, and reproductive health services specifically designed for South African women. Zoie addresses a significant gap: women’s health needs in South Africa are routinely underprioritized by a public health system under severe resource constraints, and private care is prohibitively expensive for most.
Honest Limitation: Women’s health digital platforms in emerging markets face a persistent challenge: reaching lower-income women who need the services most, not just urban professionals with the digital literacy and smartphone access needed to navigate health apps.
Rology
Rology is a teleradiology platform that connects African radiologists with hospitals that lack on-site specialists, using AI to assist with preliminary scan reading and prioritisation. It operates across South Africa, Egypt, and broader African markets, addressing the acute radiologist shortage that affects public hospital imaging departments throughout the continent.
The model is practically powerful: AI performs preliminary reads and flags urgent findings, and human radiologists then review flagged cases with the AI’s preliminary analysis as a starting point. Consequently, a radiologist supported by Rology’s AI layer can review significantly more scans per day than would be possible through manual reading alone, multiplying the effective radiology workforce without requiring more radiologists to be trained.
Honest Limitation: Rology is an AI-augmentation tool, not an AI-replacement tool; it relies on a human radiologist in the loop for review. In the very lowest-resource settings where radiologists are entirely absent, the model cannot function.
GoodX Healthcare

GoodX Healthcare is South Africa’s most widely deployed practice management platform for independent medical practitioners, used by thousands of GPs and specialists nationwide. It integrates AI for administrative efficiency: automated billing, clinical note generation, appointment management, and patient communication.
While its impact is less dramatic than diagnostic AI, the efficiency gains it delivers are real and measurable. Administrative burden is a primary driver of clinician burnout globally, and South African private practitioners are not immune. Furthermore, reducing administrative overhead means clinicians spend more time with patients, a health outcome that doesn’t appear in any app’s metrics but matters enormously in practice.
Honest Limitation: GoodX’s AI is administrative rather than clinical; it improves practice efficiency but doesn’t extend diagnostic reach or enable care in underserved communities.
South Africa Ecosystem Snapshot
South Africa’s AI healthtech story is shaped most immediately by two policy developments. The National Health Insurance (NHI) Bill (signed into law in 2024 and currently being challenged in court) would create a single-payer public health system, representing the largest public health procurement opportunity in African history.
If it proceeds, every digital health vendor with South African public sector capability is positioned for significant growth. Additionally, SAHPRA is developing specific evaluation pathways for AI-based medical devices, a regulatory development that, once complete, will significantly reduce the uncertainty that currently slows AI health product approvals.
Cross-Cutting Themes: What the Best African AI Healthtech Companies Share
Looking across these three markets, six characteristics define the companies with the most genuine traction.
Constraint-First Design
Every company with significant patient reach built its core product for the lowest common denominator of connectivity, literacy, and infrastructure, not for ideal conditions. Jacaranda Health chose SMS. Ubenwa chose audio.
Vula Mobile chose the existing smartphone camera quality. This design philosophy produces tools that are more robust and more universally applicable globally than tools designed for resource-rich environments.
Mobile-First Delivery

SMS, USSD, and lightweight app interfaces reach populations that desktop or high-bandwidth solutions cannot. 78% of city hospitals now offer video visits, and rural patients use telemedicine 52% more than before, but the companies reaching the deepest rural populations are those that are designed for feature phones and intermittent connectivity, not those that assume smartphone access.
Community Health Worker Integration
The most effective platforms (Jacaranda Health, Ilara Health) work with community health workers rather than bypassing them. CHWs are the last mile that no algorithm can fully replace. They carry social trust that no app can build from scratch.
Government Partnership Strategy
The companies with the most patient reach have all secured integration with government health programs. Private-only plays hit a ceiling in African health markets; the populations with the greatest need are in the public system, and reaching them requires public-sector alignment. Consequently, a government contract is not just a revenue stream in African healthtech; it’s the pathway to the impact that justifies the mission.
B2B and B2G Revenue Models
Direct-to-consumer health tech at prices sustainable for a startup doesn’t work when your target user earns $5 per day. The most viable African health AI businesses sell to hospitals (Helium Health), to governments (Jacaranda Health), or to clinics (Ilara Health), not directly to patients. Furthermore, this model aligns better with the realities of African healthcare economics than consumer subscription models imported from Silicon Valley.
Data Sovereignty Awareness
The best companies are building data infrastructure that keeps African health data on African servers and within African regulatory frameworks, a deliberate choice that reflects both ethical commitment and the growing regulatory expectation from NAFDAC, Kenya’s data protection authority, and South Africa’s POPIA.
At-a-Glance: Key AI Healthtech Startups Across Nigeria, Kenya & South Africa

Startup | Country | Core AI Application | Key Reach | Funding Stage |
🇳🇬 Nigeria | Hospital management + EHR AI | 500+ health facilities | Series B | |
🇳🇬 Nigeria | Newborn cry diagnostics | Clinical deployment; Gates-backed | Early stage | |
🇳🇬 Nigeria | Chronic disease home monitoring | Urban Nigeria | Pre-seed ($1.4M) | |
🇳🇬 Nigeria | Pharma supply chain AI | 1,500+ pharmacies | Series A ($12M) | |
🇳🇬 Nigeria | AI-assisted diagnostic centres | Tier 2/3 Nigerian cities | Series A | |
🇰🇪 Kenya | AI diagnostic devices for clinics | 3,000+ clinics | Series A | |
🇰🇪 Kenya | AI maternal health (PROMPTS) | 500,000+ mothers reached | Grant + equity | |
🇰🇪 Kenya | AI telemedicine + CV screening | Kenya, Uganda, Tanzania | Growth stage | |
🇰🇪 Kenya | AI emergency dispatch | Nairobi-focused | Early stage | |
🇿🇦 South Africa | AI radiology and diagnostics | SA public hospitals | Growth stage | |
🇿🇦 South Africa | AI specialist referral | 5,000+ healthcare workers | Growth stage | |
🇿🇦 South Africa | AI women’s health platform | South African women | Early-growth | |
🇿🇦 South Africa | AI teleradiology | South Africa, Egypt, Africa | Growth stage | |
🇿🇦 South Africa | AI practice management | Thousands of SA practitioners | Mature |
The Investment and Funding Landscape
The funding picture for African AI healthtech in 2026 is more nuanced than either the optimistic or the pessimistic headline narratives suggest. Here’s what you need to understand before drawing conclusions from the numbers.
Healthtech in Africa raised $224 million in equity funding in 2025, a 232% year-on-year increase, crossing the $200 million threshold for the first time since the 2021-2022 boom. That growth rate, in a normalised rather than speculative market, is the most reliable indicator of sector momentum available.
The African digital health market was projected to surpass $9.3 billion in value by 2030, attracting substantial investment from corporate venture capital, private equity, and strategic partnerships between multinational corporations and local startups. Additionally, Meta’s Llama Impact Accelerator is targeting AI health startups specifically in Nigeria, Kenya, South Africa, and Senegal; the kind of big-tech structural support that signals sector legitimacy.
The investors writing meaningful cheques include Leapfrog Investments, the Gates Foundation, the Wellcome Trust, British International Investment (formerly CDC Group), and the IFC. The funding gap that matters most is at the growth stage.
Concentration in the Big Four markets: Kenya, Nigeria, South Africa, and Egypt, captures around 83% of startup funding, suggesting that healthtech innovation in other regions faces greater funding challenges. Within those markets, seed and Series A are increasingly accessible.
Series B and beyond remain genuinely difficult. Most African healthtech companies plateau at the growth stage because patient capital is scarce, making it difficult to bridge the gap from a proven product to national-scale deployment.
Challenges and Honest Limitations Facing African AI Healthtech

No guide worth reading omits this section. The challenges are real, and you need to understand them before drawing any conclusions about the sector.
Regulatory Fragmentation
This is the defining operational challenge. Africa’s 54 regulatory environments mean that a product approved in Nigeria has no pathway recognition in Kenya, and vice versa.
Regulatory frameworks for AI and healthtech vary widely across African countries, creating compliance challenges. Nigeria’s framework is evolving, Kenya has sandbox mechanisms, but many markets lack clear guidelines. For a startup with a validated AI diagnostic tool, the cost of navigating multiple-country regulations can exceed the cost of building the product itself.
Data Scarcity for African Populations
This creates a structural AI quality problem. African health data is systematically underrepresented in global AI training datasets. Models trained on European or American patient data often perform measurably worse for African patients.
There is very sparse to no data regarding the effectiveness of AI solutions in Kenya and other African countries, and published validation studies are rare. Consequently, building AI that reliably works for African populations requires African data, which most companies don’t yet have at the scale needed for robust model training.
Connectivity and Power Infrastructure Gaps
These gaps limit reach to the populations most in need. Power cuts hit 40% of rural clinics daily, stopping apps and devices cold. Rural internet coverage sits at 30% across the continent. Any AI health tool that requires consistent connectivity or reliable power is architecturally excluded from reaching the most underserved communities.
Brain Drain
This is the talent challenge that nobody wants to name directly. African AI and healthtech talent is actively recruited by US, UK, and European tech companies at salaries that African healthtech startups cannot match. The result is an ecosystem that produces exceptional talent that it struggles to retain, a constraint that limits the speed of product development and company building in ways that funding alone cannot fix.
Trust and Clinical Adoption
remain real barriers. Clinician adoption of AI health tools requires demonstrated accuracy in African populations, not just impressive global benchmark numbers. The best companies are investing in African clinical validation studies precisely because they understand that a paper showing 94% accuracy on a European dataset does not automatically translate into clinician trust in Lagos or Nairobi.
For the broader context of AI development across the continent, including the infrastructure and talent challenges that shape what’s possible in healthtech specifically, our AI in Africa guide provides essential background. Additionally, our comparison of AI adoption across Africa and India reveals how constraint-first design principles (pioneered in health contexts) are influencing AI development globally. Furthermore, our African fintech startups landscape provides crucial context for understanding how payment infrastructure, embedded finance, and digital identity (all fintech outputs) are enabling African health AI to reach patients at scale.
What to Expect From African AI Healthtech by 2027–2028

The next two years will be shaped by several converging forces that you should understand before making any investment, partnership, or market entry decisions.
South Africa’s National Health Insurance
This is the single largest policy uncertainty in African healthtech. If the NHI proceeds (it is currently being legally challenged), it creates the continent’s largest public health procurement opportunity for digital health vendors.
Every company with South African public sector integration is watching this development closely. The outcome will reshape the South African health AI market more profoundly than any single product launch.
African Large Language Models for Healthcare
These models represent the most consequential near-term AI development for patient-facing health tools. Lelapa AI’s VulaBula API enables patients to describe symptoms in African languages, while InkubaLM allows advanced AI diagnostics to run on low-resource hardware in rural clinics.
Language models trained on African health data in African languages, being developed by Lelapa AI, Masakhane, and others, will enable patient-facing AI health tools to reach populations that current English-first models cannot serve. Consequently, our AI in Africa category is tracking these language model developments closely as they intersect with the health sector.
Embedded Health Finance
This is the next layer of infrastructure. Insurance, credit, and health payments are increasingly being bundled on a single mobile platform; M-Pesa’s integration with health payment rails in Kenya is the most advanced expression of this trend. As mobile money infrastructure deepens, the friction of paying for health services decreases, increasing the utilisation of digital health tools across all income levels.
Consolidation
This will reshape the startup landscape. Larger platforms will absorb point solutions; Helium Health’s earlier absorption of Kangpe is the template. By 2028, expect three to five dominant health platform companies across the three markets profiled here, each having consolidated multiple specialised tools into integrated ecosystems.
Global Expansion of African-Built Tools

It is already beginning. Constraint-first design means African health AI products are increasingly relevant for Southeast Asia, Latin America, and underserved communities in developed markets. The tools built to work on basic phones with intermittent connectivity and no specialist availability are precisely the tools that work in the underserved communities of Jakarta, São Paulo, or rural Alabama.
FAQs
Each leads in a different dimension. Nigeria has the highest concentration of AI health startups by volume, driven by its 220 million population and the depth of its startup ecosystem. Kenya has the most mature regulatory environment and the most evidence-backed deployments. Jacaranda Health’s 500,000+ mother reach and Ilara Health’s 3,000+ clinic network are standout metrics. South Africa has the most developed healthcare infrastructure and the most sophisticated enterprise AI health tools. For investment, Kenya offers the most regulatory certainty. But, for the scale of opportunity, Nigeria is unmatched. And, for enterprise readiness, South Africa leads.
In specific, well-defined applications, maternal health SMS guidance, newborn cry diagnostics, community health worker workflow digitisation, and African-built AI health tools are globally leading. They are not leading because African engineers are better than their global peers, but because African founders have built for constraints that produce more robust, more universally applicable tools. In broader AI capability (training data scale, compute access, regulatory certainty), African health AI is behind. The gap is closing, but it is real and honest to name it.
By patient reach, Jacaranda Health’s PROMPTS system (over 500,000 mothers reached with personalised maternal health guidance) is the most scalable patient-facing deployment. However, by clinical significance, Ubenwa’s birth asphyxia diagnostic tool addresses one of the most acute preventable causes of newborn death. By infrastructure depth, Helium Health’s 500+ facility network creates a data and clinical management layer that benefits every patient seen at those facilities. Impact is multidimensional in this sector; there is no single answer, and that’s actually evidence of a maturing ecosystem.
Conclusion

The companies profiled in this article are not prototypes. They are production systems deployed in real hospitals, clinics and communities, with real patients whose health outcomes depend on whether the technology works as promised. Helium Health is processing clinical records for half a million patients across West Africa. Jacaranda Health has reached over 500,000 Kenyan mothers with personalised guidance that reduces maternal complications.
Ilara Health has put AI-assisted diagnostics inside 3,000 Kenyan clinics that had none before. Envisionit Deep AI is reading scans in South African public hospitals where no radiologist works full-time. These are not pilot projects awaiting scale. They are the first chapter of a healthcare transformation that is already underway, already funded, and already producing measurable outcomes. Furthermore, the $224 million in equity funding raised by African healthtech in 2025, a 232% year-on-year increase, tells you that the investment community has recognised what the health data is already showing.
The honest picture includes the limitations: regulatory fragmentation, data scarcity, brain drain, and the persistent challenge of reaching the most underserved populations within already-underserved markets. These are real, and they will not be solved by a single funding round or a single policy announcement. What they will be solved by is exactly what you’re watching happen across Nigeria, Kenya, and South Africa right now: founders who understand the problems from the inside, investors who understand that patient capital is required, regulators who are building frameworks rather than barriers, and technologies that were designed for constraint rather than pretending it doesn’t exist. Additionally, for the broader AI tools and innovation context shaping what’s technically possible in African healthtech, our AI Unboxed section covers global model and tool developments that African builders are deploying and adapting.
Africa’s healthcare AI story is being written right now, and the people writing it deserve your full attention. Head to YourTechCompass.com to stay current on the African tech innovations that are reshaping health, finance, and daily life across the continent.


